Full Mouth Reconstruction
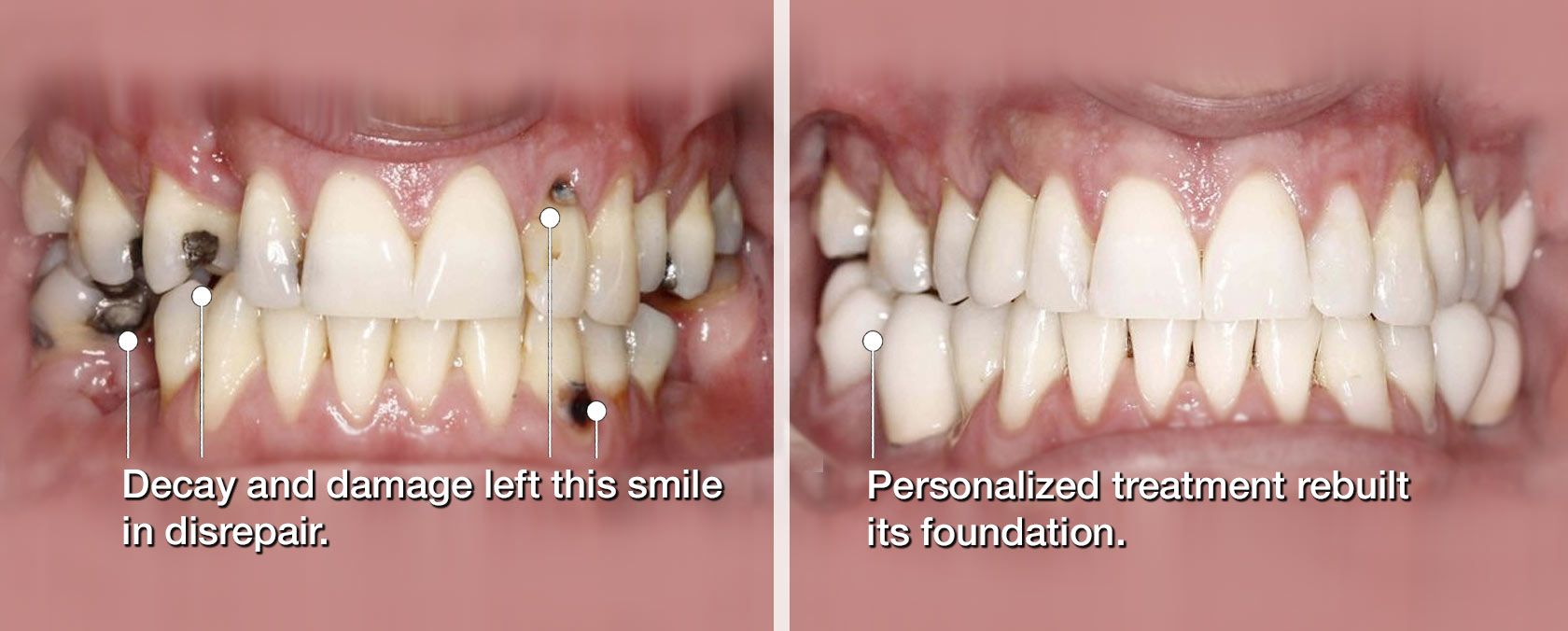
Extensive dental damage, decay, and tooth loss can impact the way your smile functions and cause you embarrassment.
An entirely customizable treatment, full mouth reconstruction can address multiple areas of your smile to restore its structural integrity.

Full mouth reconstruction is the best way to address many concerns simultaneously.
- Eliminate Your Risk of More Widespread Tooth Loss
When left unaddressed, dental decay and infection can spread to other areas of your smile. Treating these concerns can protect remaining teeth and the shape of your jaw.
- Treatment Can Have Extraordinary Aesthetic Benefits
Full mouth reconstruction is designed for your smile.
Your surgeon considers the shape of your face, the
position of your jaw, and the alignment of your teeth for beautiful results.
- Better Health, Better Function, Better Life
Missing teeth can make it difficult to chew, and patients with tooth loss often sacrifice healthy food as a result. Treatment can make it easier to eat the foods you need and love.
Design a Plan Just for You
When designing your treatment, consider all of the restorative solutions available. Dental implants can replace missing teeth, periodontal therapy can improve the health of your gums, and fillings can repair cavities. If you have temporomandibular joint disorder, also known as TMJ disorder or TMD, treatment can relieve discomfort and even protect your teeth from excessive wear and tear. You can incorporate any number of procedures into your unique treatment plan.
How can I afford such a comprehensive treatment?
You, your dentist, and your oral surgeon can work together and carefully select the restorative procedures to include in your plan, ensuring treatment meets your budget.
Financing is often available, and you may also stage treatment to make it more affordable.
Keep in mind that since this type of care is primarily restorative, insurance may cover all or part of each procedure.
How long does treatment take?
The length of your treatment will depend on the procedures you choose to include. Sometimes, your dentist or surgeon can perform more than one procedure in a single visit to expedite your treatment.
- Filling or Bonding | 1 Day
- Periodontal Therapy | Up to 1 Week
- Crown or Bridge | 2 Weeks
- Dental Implant | 3 - 6 Months
- Bone Grafting | 6 - 9 Months
- Sinus Lift | 6 - 9 Months
With a full mouth reconstruction, no case is too complex...
Fequently asked questions.
Many general dentists offer full mouth reconstruction. If your dentist does not provide comprehensive full mouth treatment plans, he or she may refer you to a colleague who does. Often, treatment involves particular procedures performed by a dental specialist, such as an endodontist, periodontist, prosthodontist, or oral surgeon. For children who have experienced oral trauma, we may recommend a pediatric dentist or pedodontist.
Often, a general or family dentist will offer full mouth reconstruction. In some cases, however, a dentist may refer a patient to a colleague for full mouth reconstruction, simply because the general practitioner believes that the patient would be better served by a doctor who has more experience and training in full mouth reconstruction.
Treatment time depends upon the scope of the treatment plan, patient compliance, and how quickly a patient recovers after procedures. After a thorough oral evaluation and discussion, your dentist should be able to provide a treatment timeframe. If you need treatment completed in a particular amount of time, be sure to let your dentist and oral surgeon know your expectations at your consultation.
Of course, you’ll have to be available for dental appointments. If your work schedule is an issue, be sure to discuss it with your dentist and oral surgeon ahead of time. Chair time required for treatment will depend on the procedures in your full mouth reconstruction treatment plan.
If your treatment plan involves oral surgery, you may need to take time off work for recovery. Tell your dentist about your work commitments so that he or she may factor that into your treatment plan.
Because each patient’s treatment plan is unique, the cost of treatment varies greatly. If finances are an issue, consider a phased treatment plan or financing. Some patient financing companies offer low- and no-interest loans for qualified applicants. You can use dental insurance and health savings accounts to help with full mouth reconstruction costs. If finances are an issue, be sure to tell your surgeon and dentist. The doctor may have the option to use dental materials and procedures that can make your treatment more affordable. Of course, less esthetic materials (metal instead of natural looking) and alternate materials (bonding instead of veneers) come with some concessions. Discuss the pros and cons of various dental materials and treatment options with your doctor before undergoing treatment.
Choices may include phased treatment or using third-party or in-house financing. Phased treatment plans allow a large treatment plan to be divided into affordable, practical segments. Third party or in-house financing may be available for qualified applicants. In some cases, low or no interest financing options exist.
No one is “too old” for good oral health and comfortable oral function. Age can, however, be an important factor in treatment planning, because elderly patients often have health issues that must be considered in a full mouth reconstruction plan. For instance, if the doctor determines that a patient may not do well during or after surgery, he or she may recommend mini dental implants, instead of traditional implants, for denture retention. Don’t allow age to keep you from a healthy mouth and comfortable oral function. A competent dentist will be able to work with you to develop an appropriate, effective treatment plan, regardless of your age.
Dental phobia is a common, and very real, problem for many patients who need full mouth reconstruction. Years of avoiding professional dental care due to dental anxiety, stress, or phobia can result in deteriorated oral health. Regardless of your oral health condition, if you don’t like dental visits, tell your dentist.
Don’t allow being afraid of the dentist to stand between you and optimal oral health.
Today, anxious dental patients have access to nitrous oxide (laughing gas), anxiolysis (oral sedation), oral conscious sedation (nitrous oxide with oral sedation), and IV sedation (intravenously administered drugs). These sedation options can make an anxious or extremely phobic dental patient find peace of mind and body during dental procedures. Don’t allow being afraid of the dentist to stand between you and optimal oral health.
With modern dental anesthetics and sedation, no dental procedure has to hurt. Your dentist will recommend the appropriate level of medication for your comfort. Some patients experience short-term oral discomfort following a procedure. Your dentist may suggest over the counter or prescription pain relievers to take after treatment, for your comfort.
Tell the surgeon if you know that you have a sensitive gag reflex, clinically known as laryngeal spasm. The surgeon can take measures to reduce your risk for gagging, and to optimize your comfort.
If you know that local anesthesia does not sufficiently numb your mouth, tell your oral surgeon during your initial consultation so that he or she can note your chart accordingly. The doctor can administer nitrous oxide, oral sedation, or oral conscious sedation to keep you comfortable during dental treatments.
Discomfort in the dental chair is a common issue, but it can be easily overcome with medication. Nitrous oxide, oral sedation, or oral conscious sedation can help you remain comfortable.
Yes. If your general dentist and surgeon believe that you would be better suited under the care of a doctor with more experience treating special needs patients, he or she may refer you to a respected colleague. Often, a surgeon administers sedation so that a special needs patient can comfortably undergo treatments for full mouth reconstruction.
The longevity of treatment results will depend greatly upon your oral health, overall health, oral hygiene, and compliance with doctor’s instructions. Dental materials are also a factor. Porcelain veneers, for instance, may last two decades or more; dental bonding to correct the same issue may only last five to ten years.
If you suffer from chronic migraines, headaches, pain in the jaw, head, neck, shoulders, or back, tell your dentist. He or she can assess your occlusion and jaw joints to determine whether TMJ disorder (TMD) is causing your symptoms and incorporate appropriate treatment into your plan.
Habitual teeth grinding is clinically known as bruxism and is a common affliction: according to the National Institute of Dental and Craniofacial Research, an estimated 10 million Americans suffer from the condition.
Over time, teeth grinding takes a toll on teeth by wearing down molars or causing chips and fractures. Therefore, bruxism should be treated so that the results of full mouth reconstruction are preserved. A simple oral appliance called a mouth guard can prevent teeth grinding, but the underlying cause should also be treated.
Children can require full mouth reconstruction. Common causes are baby bottle mouth (decay across front teeth) and injury. A child who needs full mouth reconstruction should see a pedodontist (children’s dentist).
Oral cancer is a serious and common disease that can affect people with no high-risk factors. If your dentist finds cause for an oral biopsy, he or she may refer you to an oral surgeon. Rest assured, your dentist will answer all your questions and explain next steps if you ask.
The oral surgeon will recommend you create a plan to get this under control prior to undergoing full mouth restoration. Your dental hygienist or dentist will suggest appropriate treatment, based on your level of gum disease. Also called periodontal disease, gum disease is a chronic condition that has no cure, but it can be treated.
Early gum disease is known as gingivitis, and few symptoms are expressed. In fact, some patients with gingivitis experience no symptoms. Treating gingivitis may simply involve changing your oral homecare routine and using special mouthwash. However, a deep cleaning may also be suggested if gingivitis has progressed.
Gum disease is a chronic condition that has no cure, but it can be treated.
Deep cleaning takes a few hours and is often performed in two visits. It involves scaling, which is removing hardened plaque (tartar or calculus) from below the gum line, and root planing, which is smoothing rough areas on teeth roots. If you have periodontitis, the advanced stage of gum disease, you may need surgery. Often, a general dentist will refer patients with periodontitis to a periodontist for treatment.
Some, not all, dentists employ lasers for minimally invasive dental and periodontal procedures. A soft tissue laser can treat periodontitis, reduce gum tissue for cosmetic purposes, and perform biopsies. Hard tissue lasers can prepare teeth for restorations, clean a tooth’s root canal, and trim bone tissue. Patients tend to heal promptly following laser surgery, and lasers offer an unparalleled level of precision.








